Do you know diet is one of the major factors affecting the outcome of Migraine? In many aggravating factors of diet plays a significant role. So, today we will compare 6 types of diet and see their role in the treatment of migraines. In conclusion, try to find the best one.
On this Page
- What is Migraine?
- How do you know its Migraine?
- How can it be managed?
- Role of diet in Migraine
- Different Diet and migraine
- Conclusion
- Frequently Asked Questions
1) What is Migraine?
Migraine usually an episodic headache associated with certain features such as sensitivity to light, sound, or movement. Above all nausea and vomiting often accompany the headache.
However, a useful description of it is a recurring syndrome of headache associated with other symptoms of neurologic dysfunction in varying admixtures.
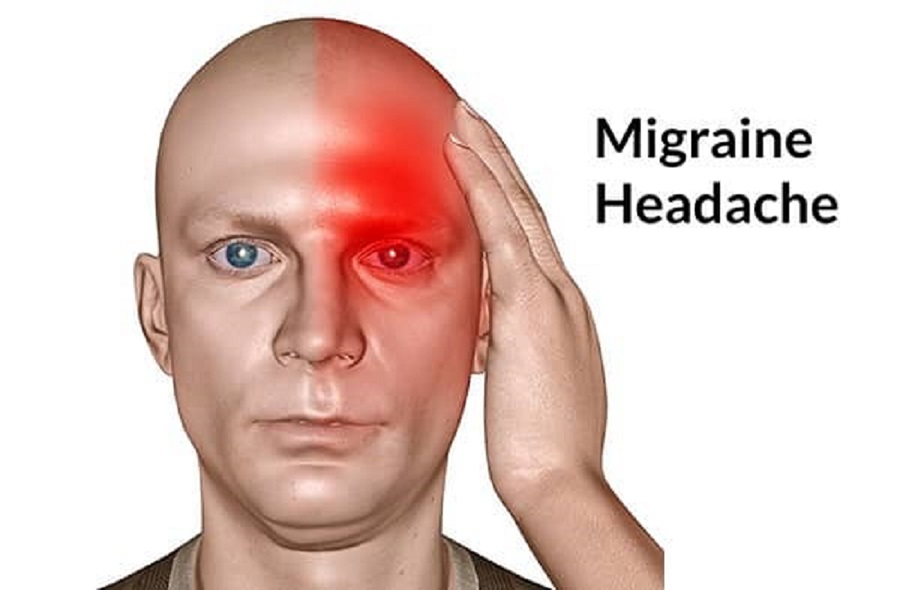
It has three phases: premonitory (prodrome), headache phase, and postdrome. In addition, each has distinct and sometimes disabling symptoms.
In addition about 20–25% of migraine people have a fourth, aura, phase. It can often be recognized by its activators, referred to as triggers.
Migraineurs are particularly sensitive to environmental and sensory stimuli. Hence migraine-prone persons do not habituate easily to sensory stimuli. This sensitivity is amplified in females during the menstrual cycle.
Headache can be initiated or amplified by various triggers, including glare, bright lights, and sounds. Similarly, other types of afferent stimulation; hunger; stress; physical exertion adds to the pain.
Above all hormonal fluctuations during menses; lack of or excess sleep; alcohol or chemicals, such as nitrates pile misery.
Knowledge of a person’s susceptibility to specific triggers can be useful in management strategies involving lifestyle adjustments. Although it is becoming recognized that some apparent triggers may in fact be part of the initial phase of the attack; i.e., the premonitory phase or prodrome.
2) How do you know its Migraine?
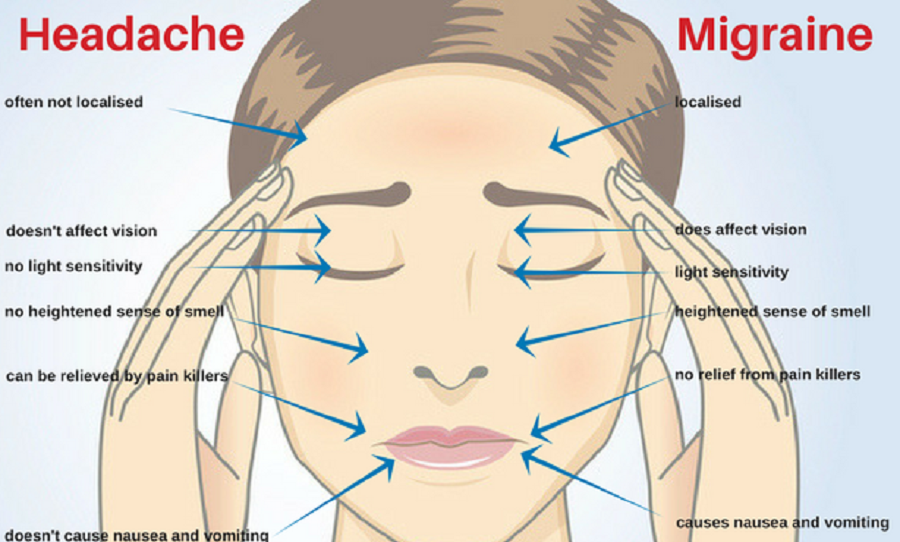
The main symptom is repeated attacks of headache lasting 4–72 h. However, no other reasonable cause for the headache is seen.
In addition also have any 2 of the following 4 things (Unilateral pain Throbbing pain, Aggravation by movement, Moderate or severe intensity and at least 1 of the following 2 things Nausea/vomiting, Photophobia, and phonophobia.
3) How can it be managed?
Certainly, there are a lot of pharmacological options available, from painkillers to a lot of therapy. But still, the best treatment is prevention.
In other words, nonpharmacologic approaches can manage some degree of migraine. When patients can identify reliable triggers, their avoidance can be useful.
Meanwhile, a regulated lifestyle, including a healthy diet, regular exercise, regular sleep patterns, avoidance of excess caffeine, above all alcohol is helpful.
In addition avoidance of acute changes in stress levels, and being particularly wary of the let-down effect is most.
4) Role of Diet in Migraine
Among lifestyle modalities, nutraceuticals and diet play a notable role in headache/migraine, and therefore adjusting one’s diet could be useful in preventing and treating headaches.
The main components of a comprehensive diet include carbohydrates, proteins, fats, vitamins, and above all ions. It is not clear whether these dietary factors prevent or provoke headache attacks. The initiation of an attack may occur following the consumption of specific food items.

Moreover, making specific dietary recommendations based on persons’ needs, and types of comorbidities could be effective in reducing the frequency of headaches or even preventing the initiation of an attack.
So far, the effects of different types of diets have been studied in relation to migraine and headache. It is thought that dietary interventions could affect headache/ migraine characteristics through a variety of mechanisms.
These mechanisms may include affecting serotoninergic dysfunction, neuronal excitability, levels of factors with a role in migraine pathogenesis (such as Calcitonin-Gene- Related-Peptide (CGRP), nitric oxide (NO), adiponectin, and leptin), brain mitochondrial function, neuroinflammation, hypothalamic function, and platelet aggregation.
For example, obesity, which is highly related to western dietary patterns, is also thought to be prevalent among headache person. It has been proposed that headaches could be improved following reducing excessive weight.
5) Different Diet and Migraine

So, here we will discuss a few dietary approaches which can be effective in migraine. We will also see which dietary approach will be good one for migraines by comparing different studies done.
Fasting and carbohydrate restricted diets (ketogenic Diet)
Carbohydrate content in KD is highly restricted which results in inducing fasting in addition to rapid weight loss and elevating metabolism of fat and thus producing ketone bodies (KB).
KD was initially designed in order to stimulate the ketotic effects of fasting. The KD was used to treat refractory epilepsy since the time of Hippocrate.

Different studies say that a modified fasting diet with 3–4 high protein/low carbohydrate (200 kcal) a day establishes ketosis. Therefore helping headache attacks disappear. Above all, this effect remains for 7 months after stopping fasting.
Low calorie Diet , Modified Atkins Diet (MAD)
Low-calorie diet (1200–1500 kcal/d) for months can result in a significant reduction in headache days and above all unhealthy medication consumption.
Some studies suggest that twenty-eight percent reaches complete remission from migraine headaches. Also, continuous improvement can be seen for 3 months after stopping a low-calorie diet.

Low glycemic diet (LGD)
In LGD, daily carbohydrate intake is restricted to 40–60 g with a glycemic index (GI) of less than 50.
So consumption of white bread, sugar, chocolate, sweets, pastries, rice, potato, corn, jams, honey, molasses, ready-made fruit juices, sugary carbohydrate drinks, watermelon, and melon are limited.
LGD carbohydrate mainly comes from legumes, vegetables, fruits, and above all, high fiber cereals. Similarly, different studies have found that there is a significant loss of headache by this diet.
Though there are lesser studies done regarding a low glycemic diet. But it is known that this diet modifies inflammatory response and hence results in decrease headache.
Low-fat diet
Restriction of fat intake to less than 20 g/d has reported a notable reduction in headache frequency, intensity, and need for unhealthy medication. A study even says that high omega-3 combined with low omega-6 diet results in higher headache improvement compared to headache patients on the reduced omega-6 diet.
Above all combination of nano curcumin and ω-3 fatty acids lowers the expression of TNF-α mRNA and serum level of TNF-α resulting in a decrease in the frequency of headache.
Elimination diet

Each headache person may have a specific trigger or a unique set of triggers. Therefore it is known that certain types of foods and beverages can act as headache triggers.
Cheese, chocolate, citrus fruit, alcohol, coffee, tomatoes, carbohydrates, leavened products, and above all red wine are foods that trigger migraine attacks.
However, Some sufferers report that specific foods only provoke headaches in combination with stress or extended physical exercise. Both conditions are identified as headache triggers and lead to the production of proinflammatory cytokines.
Therefore, it seems that applying elimination diets in headache patients with food sensitivities could be effective in preventing migraine attacks, though more studies are needed.
Similarly, some people may also be sensitive to other triggers like histamine, which is related to the impairment of detoxification caused by a low activity of di-amino-oxidase.
Histamine thus may play an additional role which should be considered in the elimination diets.
Low sodium diet
so, According to a different study, there might be a negative relationship between blood pressure and headache occurrence. Therefore, it may be logical to anticipate that dietary interventions that reduce blood pressure, could also lower headache occurrence.
However, available evidence on sodium intake in relation to headache has mainly focused on monosodium glutamate (MSG). Therefore, the current data on the effects of dietary sodium intakes on headache characteristics is not conclusive yet.
You can also read My other blog:
Health and hygiene | BJP – bartan jhadu poocha 10 Female secret advice:
House party:10 ways of organizing an awesome house party
Healthy Diet Patterns You Should Follow in 2020 for health
Everything You Want To Know About Low Carbohydrate Diet
Healthy Breakfast Recipes To Boost Your Morning
How to deal with stress | Secret Phycology of Doctors.
TOOTHACHE: 7 DENTAL HYGIENE TO RELIEF FROM IT
6) Conclusion
So, different nutritional interventions are effective in migraine and their associated symptoms. Similarly, there are different types of diets that are thought to increase migraine headaches.
For instance, KD and MAD might play a role in neuroprotection, mitochondrial function, and energy metabolism, compensating serotoninergic dysfunction, decreasing the CGRP level, suppressing neuroinflammation, and CSD.
so, A low glycemic diet helps to prevent headaches/migraines by increasing the inflammatory state. Moreover, obesity and headaches especially migraines could be attributed to each other through mechanisms like inflammation, and irregular hypothalamic function.
Thereby, applying dietary strategies for weight loss may also cure headaches/migraines. Another important dietary intervention that might be effective in headache/migraine improvement is related to the balance between the intake of essential fatty acids, omega-6, and omega-3.
Therefore, these dietary approaches could affect inflammatory responses, platelet function, and regulation of vascular tone.
Regarding the elimination diet, it could mostly be effective in migraine patients with food sensitivities to prevent headaches.
7) Frequently Asked Questions
Ans. 1) so, Migraines are a temporary change in brain physiology that occurs in normal brains in response to certain triggers. therefore, These changes in brain physiology can result in multiple symptoms, the most notable of which is usually a headache.
Ans. 2) Diet, lifestyle, and hormonal factors trigger migraines. With rare exceptions, it is never any one thing that causes a migraine attack but is rather the culmination of many different factors that “flip” the brain’s migraine switch.
Ans. 3) Migraines are primarily triggered by dietary, lifestyle, and hormonal factors. With rare exceptions, it is never any one thing that causes a migraine attack but is rather the culmination of many different factors that “flip” the brain’s migraine switch.
Ans. 4) MRIs are typically done in specific circumstances in which the cause of your headaches is somewhat uncertain, and your doctor feels it necessary to exclude other possible causes of headaches. In most cases of migraines, however, MRIs are not necessary.
Ans. 5) It’s important to have an effective strategy for migraine relief and be ready to employ that strategy whenever needed. Fortunately, medications to relieve a migraine attack have improved greatly over the past couple of decades, so there are many options. For some, over the counter remedies work well. For others, only prescription medications will work.
